You already know stress can make your heart race, your mind spiral, or your body shut down. What many people miss is that these reactions may be nervous system patterns—not personal failures. In this guide, you’ll learn what polyvagal theory is, how its three states work, and practical ways to regulate your body and mind.
Key Takeaways
- Polyvagal theory explains how the nervous system shifts between connection, mobilization, and shutdown states in response to perceived safety or threat.
- Ventral vagal states support calmness, social connection, and flexible thinking.
- Sympathetic activation prepares the body for fight or flight and can feel like anxiety, urgency, or irritability.
- Dorsal vagal shutdown can involve numbness, collapse, fatigue, or disconnection when stress feels overwhelming.
- Regulation skills such as breathing, movement, grounding, and safe relationships can help the body return to balance.
- Polyvagal theory is widely used in trauma-informed practice, but some scientific aspects remain debated.
- Nervous system awareness can improve self-understanding and guide healthier coping strategies.
What Is Polyvagal Theory and Why Is It Important?
Polyvagal theory is a framework that describes how the autonomic nervous system responds to cues of safety, danger, and life threat. It was introduced by neuroscientist Stephen Porges in the 1990s. The theory suggests your body constantly scans the environment for signals that tell it whether to connect, protect, or shut down.
First, the theory focuses on the autonomic nervous system, which controls automatic functions like heart rate, breathing, digestion, and stress responses. For example, when you feel safe with a trusted friend, your body may relax without conscious effort. how the nervous system works
Second, polyvagal theory matters because it reframes many emotional struggles. Instead of asking, What is wrong with me? you can ask, What state is my nervous system in right now? That shift often reduces shame and increases self-compassion.
Third, this framework is popular because it connects mental health with body sensations. Many people notice anxiety in the chest, shutdown in the limbs, or calmness in the breath before they can explain it with words.
Quotable insight: Nervous system states often change before conscious thoughts do.
Quotable insight: Safety is not only a thought; it is also a body experience.
Who Created Polyvagal Theory and What Does It Claim?
Polyvagal theory was created by Stephen Porges and claims that the vagus nerve plays a central role in emotional regulation, connection, and defensive responses. The vagus nerve is a major nerve linking the brain and body.
Moreover, the theory proposes that humans have layered survival responses. When connection works, the body stays socially engaged. When danger appears, the body mobilizes. When overwhelm feels extreme, the body may immobilize.
For example, imagine giving a presentation. If you feel supported, you may speak clearly. If you feel threatened, your heart may pound. If the stress feels unbearable, your mind may go blank.
At the same time, many clinicians use the theory as a practical map, even when they debate some biological details. That distinction matters: a model can still be useful even when parts remain contested.
Why Does Polyvagal Theory Matter for Stress, Anxiety, and Relationships?
Polyvagal theory matters because it helps explain why stress affects emotions, relationships, and behavior so quickly. It gives people language for patterns they already experience.
First, anxiety often feels less mysterious when you understand activation states. Racing thoughts, irritability, urgency, and muscle tension may reflect a mobilized nervous system rather than a character flaw. stress management techniques
Second, relationships improve when people understand state changes. A partner who goes silent may be shut down, not uncaring. A parent who snaps may be overloaded, not intentionally cruel. This awareness can reduce blame.
Third, emotional regulation becomes more practical. Instead of forcing positive thinking, you can use body-based tools that help the nervous system feel safer first.
Stress remains common worldwide. The World Health Organization has repeatedly identified stress-related mental health concerns as a major public health issue — Source: WHO, 2023.
Quotable insight: Understanding your state can be the first step toward changing your response.
Quotable insight: Regulation often works better than self-criticism.
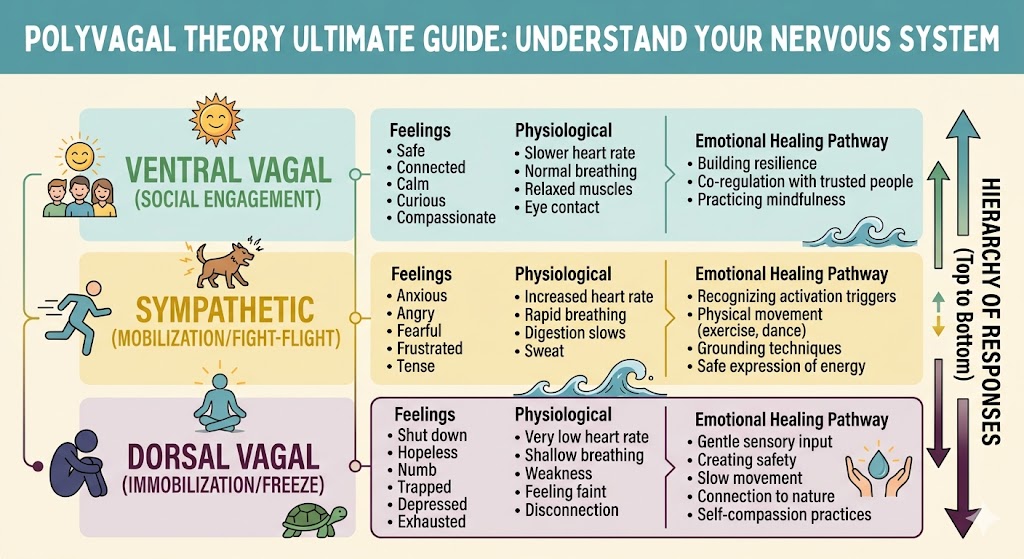
What Are the Three Polyvagal States?
The three polyvagal states are ventral vagal, sympathetic, and dorsal vagal. These states describe broad patterns of connection, mobilization, and shutdown.
| State | Main Function | Common Feelings | Typical Behaviors |
|---|---|---|---|
| Ventral Vagal | Safety & connection | Calm, present, curious | Socializing, learning, problem-solving |
| Sympathetic | Fight or flight | Anxious, angry, urgent | Overworking, arguing, escaping |
| Dorsal Vagal | Shutdown / freeze | Numb, tired, disconnected | Withdrawal, collapse, avoidance |
How Does the Ventral Vagal State Affect Mental Health?
Ventral vagal activation supports calmness, social connection, and flexible problem-solving. This is the state many people describe as grounded and emotionally available.
For example, you may listen better, digest food more comfortably, and recover from stress faster. Research consistently links supportive relationships with better mental and physical health — Source: Harvard Adult Development Study, 2023.
In addition, this state supports learning and creativity. When your body feels safe, your brain can devote more resources to growth rather than survival.
What Does Sympathetic Fight or Flight Feel Like in Daily Life?
Sympathetic activation involves the body’s mobilization response, commonly known as fight or flight. It prepares you to act quickly.
For example, you may feel restless, tense, reactive, or unable to sit still. Some people become productive and busy. Others become angry or panicked. signs of burnout and chronic stress
That being said, sympathetic activation is not bad. It helps you meet deadlines, exercise, or respond to real danger. Problems usually appear when the body stays activated for too long.
What Is Dorsal Vagal Shutdown and How Can You Recognize It?
Dorsal vagal shutdown involves immobilization responses such as numbness, collapse, or disconnection under overwhelming stress. This can happen when the system believes action will not help.
For example, a person may feel exhausted, emotionally flat, foggy, or detached from others. They may cancel plans, stare at screens for hours, or struggle to initiate simple tasks.
Importantly, shutdown is also a survival response. It is not laziness. It is the nervous system trying to conserve energy when life feels too much.
How Does Polyvagal Theory Work in Daily Life?
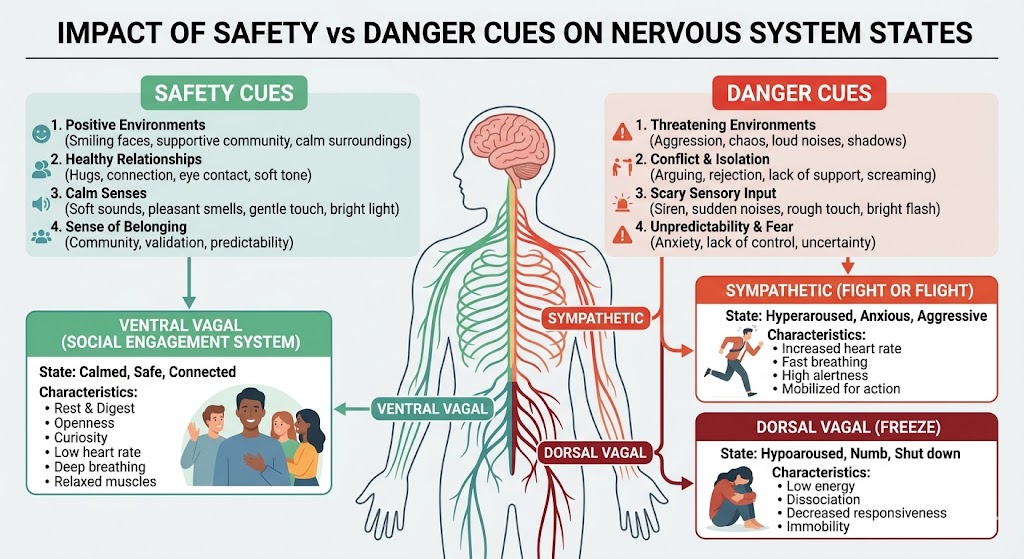
Polyvagal theory works in daily life by showing how cues of safety or danger shape mood, behavior, and body sensations. These cues can be external or internal.
First, external cues include tone of voice, facial expressions, conflict, deadlines, crowded spaces, or supportive touch. For example, a harsh email may spike tension before you even finish reading it.
Second, internal cues include hunger, poor sleep, pain, illness, or memories. Sleeping less than recommended amounts is linked with poorer emotional regulation and stress resilience — Source: CDC, 2024. mindfulness for beginners
Third, daily regulation often means changing the cue, not just changing the thought. Softer lighting, hydration, a calm voice, or a short walk can shift the body faster than endless analysis.
How Does Polyvagal Theory Explain Trauma Responses?
Polyvagal theory explains trauma responses as nervous system adaptations to overwhelming experiences. The body learns protective patterns that may continue long after danger has passed.
First, trauma can create chronic sympathetic activation. A person may stay hypervigilant, easily startled, or unable to relax. For example, they may scan rooms for exits or expect conflict.
Second, trauma can create chronic shutdown. A person may feel numb, disconnected, or emotionally distant. For example, they may avoid closeness because closeness once felt unsafe.
Third, triggers often make more sense through this lens. A smell, sound, tone, or relationship dynamic can reactivate old body memories quickly. how trauma affects the body
Trauma exposure is widespread. Many adults report at least one significant traumatic event in life — Source: National Council for Mental Wellbeing, 2023.
Quotable insight: Trauma responses are learned protections, not permanent identities.
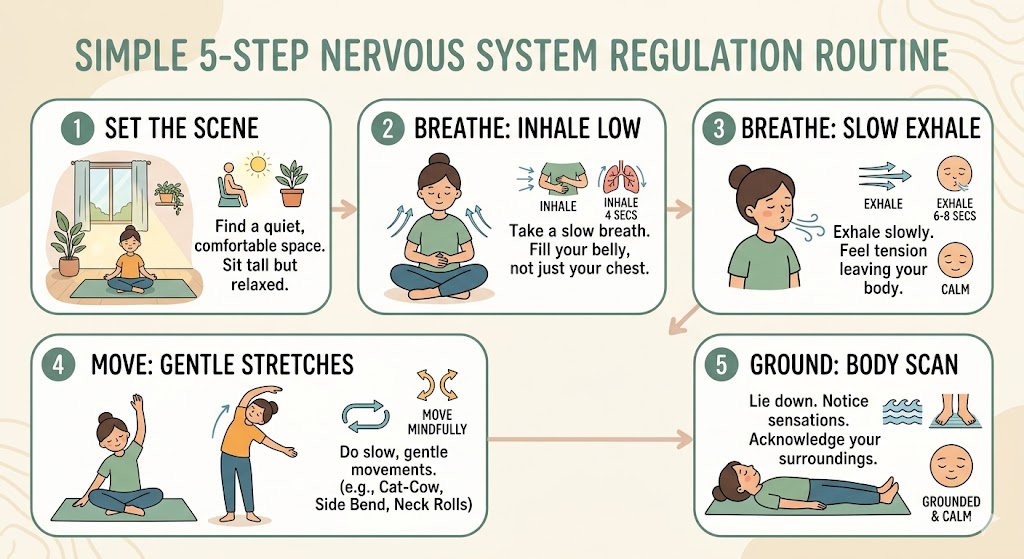
How Can You Regulate Your Nervous System Using Polyvagal Techniques?
Nervous system regulation involves practices such as slow breathing, movement, grounding, and supportive social connection that help restore a sense of safety. Small, repeated actions often work better than dramatic one-time fixes.
1. Slow Breathing
Slow breathing is a fast-access regulation tool that can reduce arousal. Longer exhales often help many people settle.
For example, inhale for 4 seconds and exhale for 6 seconds for two minutes. best breathing exercises for anxiety
2. Grounding
Grounding redirects attention to the present moment through sensory awareness. It is useful when thoughts spiral.
Try the 5-4-3-2-1 method:
- 5 things you see
- 4 things you feel
- 3 things you hear
- 2 things you smell
- 1 thing you taste
grounding techniques for panic
3. Movement
Movement helps complete stress energy. Gentle walking, stretching, shaking out the arms, or dancing can help discharge activation.
For example, a 10-minute walk after a stressful meeting may reduce tension faster than sitting and ruminating.
4. Co-Regulation
Co-regulation is the calming effect of safe connection with another person. Humans regulate in relationships.
For example, talking with a trusted friend, hugging a loved one, or hearing a warm voice can help the body settle. healthy relationship communication tips
5. Sleep and Sensory Care
Sleep and sensory habits strengthen baseline resilience. Consistent sleep, sunlight, hydration, and lower overstimulation support recovery. sleep habits for stress recovery
Is Polyvagal Theory Scientifically Proven or Controversial?
Polyvagal theory is influential and clinically useful, but some scientific claims remain debated. This balanced view is important.
First, many therapists and clients find the framework highly practical. It offers understandable language for body-based stress responses and supports trauma-informed care.
Second, some researchers question whether the theory oversimplifies autonomic pathways or overstates specific vagus nerve distinctions. Scientific progress often includes debate, refinement, and reinterpretation.
Third, you do not need to treat it as absolute truth to benefit from useful practices. Slow breathing, movement, sleep, and social support are supported by broader evidence beyond the theory itself. science-backed relaxation methods
Quotable insight: A model can be helpful even while parts of it are revised.
Quotable insight: Practical benefit and scientific debate can exist at the same time.
How Can Therapists and Coaches Use Polyvagal Theory in Practice?
Therapists and coaches use polyvagal theory as a roadmap for noticing states, building safety, and choosing regulation tools. It often guides conversations and interventions.
First, therapists may help clients track triggers, body sensations, and recovery patterns. For example, they may ask, What happened in your body before the panic started?
Second, coaches may use the framework for workplace stress and performance. A client who procrastinates may need regulation before productivity tactics.
Third, parents and couples can use it to repair conflict. Instead of escalating, they can pause, regulate, and return when both people feel safer.

What’s Next: How Do You Build a Nervous System Regulation Plan?
A nervous system regulation plan is a simple system for noticing triggers, using tools, and recovering faster over time. Consistency matters more than perfection.
Step 1: Track Your Patterns
Write down:
- What triggered you
- What you felt in your body
- Which state you noticed
- What helped you recover
Step 2: Build Safety Cues
Create a personal list:
- Music that calms you
- Supportive people
- Places that feel peaceful
- Sensory tools like blankets or scents
Step 3: Practice Daily Micro-Regulation
Use 2–5 minute habits:
- Morning breathwork
- Midday stretch
- Evening screen break
- Gratitude or journaling
Step 4: Get Support
If symptoms feel intense or persistent, seek professional help. [Internal link: “therapy options for anxiety” → suggested target page/topic]
Step 5: Protect Recovery
Conclusion
Polyvagal theory offers a practical lens for understanding stress, connection, and shutdown responses. Your reactions are often adaptive patterns shaped by experience, not evidence that you are broken. By learning your states and practicing small regulation skills, you can gradually build more calm, flexibility, and resilience.
Written by Suraj 5+ Blogger — SEO content writer and educational wellness researcher focused on evidence-aware, reader-first health content.
Reviewed by Editorial Review Team — Mental health and behavioral science content reviewers with expertise in psychology communication and wellness education.
Disclaimer: This article was initially drafted using AI assistance. However, the content has undergone thorough revisions, editing, and fact-checking by human editors and subject matter experts to ensure accuracy.